Home
May 18th, 2019 by leahtourtellotte
Posted in Uncategorized|
I completed 4 weeks in Haiti and now I’m back in the US. The change has been hard. I can’t help but keep comparing the condition there and here. We are so lucky here and I take it for granted every day. I have affordable electricity all of the time. I have water that I can drink practically anywhere and hot water whenever I want. I have wifi or 4g everywhere. I can go to happy hours and all you can eat restaurants in a variety of cuisines. I’ve already gone to see Avenger’s Endgame. To live just seems easier here.
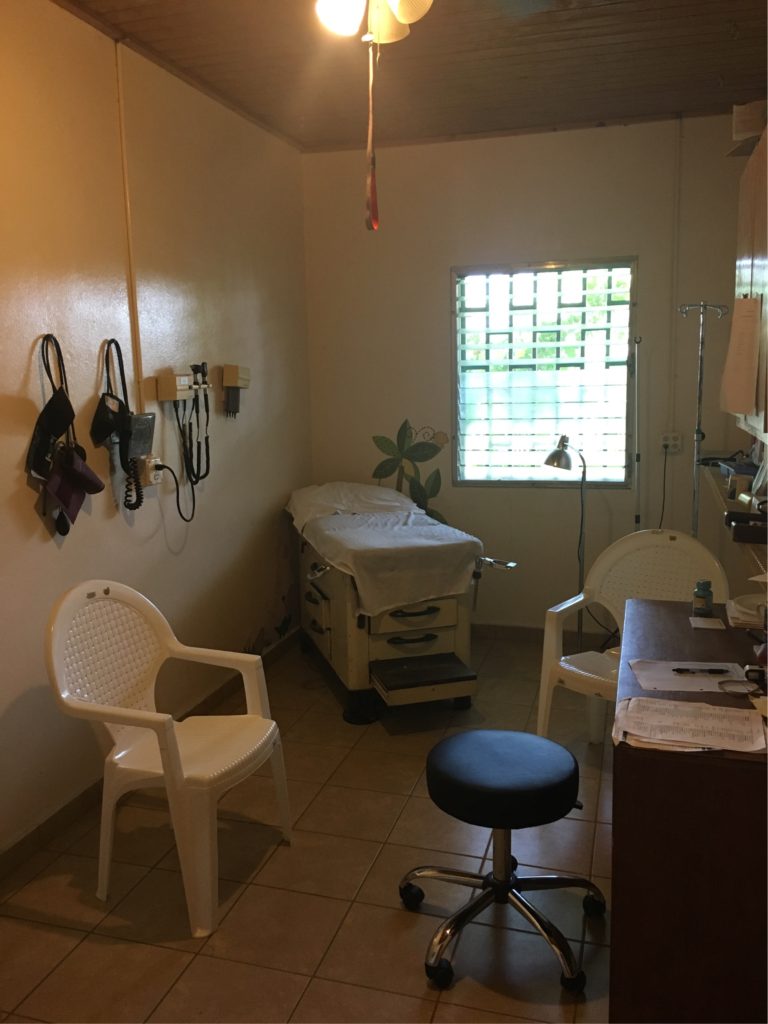
I went on a tour the other day of our micro and chemistry labs at Eisenhower and thought back to the one room lab in Haiti. No cultures. No fancy machines. Labs that go in and out of availability. Numbers that print out on pieces of paper that like look old school cash register receipts. Here blood literally goes through one machine that takes it to other machines depending on the test and you can see little mechanical arms pipette chemicals and numbers result on computer screens. Cultures get stacked up in incubators. A machine runs analytics that can identify the organism. What a difference!
I had a likely TB patient the other day. Airborne precautions and N95 masks of course! In Haiti, we had run out of PPDs. Now not only can I do a PPD, I can do a quantiferon gold and AFB smears. I can also rule out other things like cocci. The chest xray has a consolidation; let’s order a CT. Now I can actually see that right upper lobe cavitating lesion. I can start RIPE right away and follow up that culture. As a clinician what I didn’t realize was how much I would miss relying on tests and imaging to make a diagnosis. In Haiti, I didn’t anticipate the anxiety I would have in questioning myself and hoping that I diagnosed appropriately.
How did I end up in what seems like a different world? And perhaps most importantly, how can these disparities be overcome so that others may live healthy and socially rewarding lives as we do?