“I have malaria!” shouted a young mother. “I as well,” declared a shivering elderly man. “My children, they all have malaria,” confirmed a distraught father, “and one died this morning!”
In response to my question, “Who has malaria?”, over 100 hands raised among the crowd of patients waiting to see me. Adding to their urgency was the increasing ricochets of distant gun fire, which at that time characterized our lives amid the Angola Civil War.
I was prepared, so I thought. Before moving to Angola, a nation in southern Africa, I diligently studied malaria and other tropical diseases at the US Army Walter Reed School of Tropical Medicine. But the sheer number of sick Angolans was far beyond my capacity to treat.
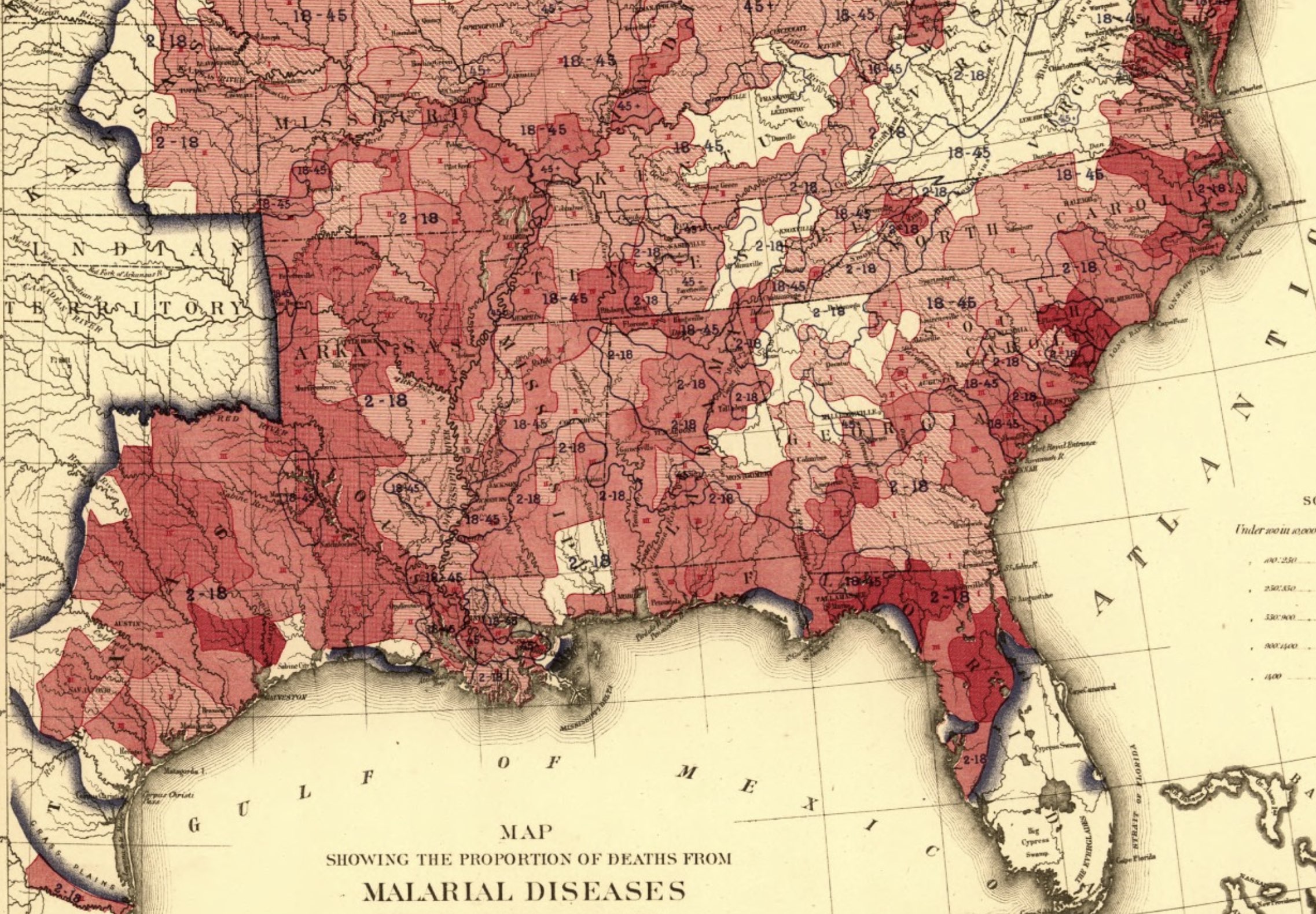
Malaria once infected Americans. This map from 1870 shows the extent of malaria deaths, particularly lethal in the warm humid climate of the south. Military commanders during both World Wars were frequently changed battle strategies because of epidemic malaria among their soldiers. Agriculture leaders often watched their crops wither because farmworkers were too feverish to harvest.
In 1947, in fact, 15,000 cases were still reported in the U.S. But by 1951, malaria was declared eliminated from the U.S. Dramatic progress! How was this possible? Major milestones include:
- In 1897 when scientists discovered that malaria parasites were transmitted to humans through the bite of Anopheles mosquitoes.
- In 1933, the Tennessee Valley Authority spearheaded malaria control by varying water levels in reservoirs that prevented mosquitoes from laying eggs.
- 1947 the National Malaria Eradication Program, a cooperative of 13 southeastern states, started spraying insecticide on the interior surfaces of rural homes that killed indoor mosquitoes.
In short, elimination of malaria from the United States was accomplished through decisive public action guided by objective science. Sure, news reports from that era describe individuals draining pools of standing water. But to combat such a widespread infectious disease, only government-guided action at scale was truly effective.
This principled approach has led to stunning progress against the greatest plagues afflicting humanity: smallpox, measles, polio, tuberculosis, diphtheria, tetanus, typhoid fever – all science-based initiatives guided by the US Center for Disease Control and Prevention.
Back in Angola, my heart raced over the dilemma of how to care for so many people with suspected malaria infection. The combatants were nearing, and the twilight grew.
Invoking the principles of triage, I personally examined those who were most ill, usually young children. I also engaged the skill of talented Angolan nurses whom I earlier trained to manage febrile illness. And, with every patient encounter we emphasized the importance of malaria control: use of bed nets, drainage of standing water, and early treatment. These are all principles we at INMED continue to entrust to our learners through the Graduate Certificate Course in International Health.
Ultimately, significant progress against malaria in the nation of Angola stalled until public action in 2002. With the end of the chaotic civil war. came greater supply of bed nets, better laboratory for diagnosis, superior medications for treatment, and public works to remove standing water.
Malaria in America and Malaria in Angola – both ultimately controlled through decisive public action guided by objective science.